Alex Schadenberg
Executive Director, Euthanasia Prevention Coalition
 |
St Paul's hospital Vancouver
|
A euthanasia lobby group has been lobbying the British Columbia (BC) government to force Catholic hospitals to provide euthanasia.
Samantha O'Neill (34), died
by euthanasia (MAiD) on April 4, 2023 after being transferred from St Paul's
hospital in Vancouver to St. John’s Hospice.
O'Neill's family argue that Samantha should have been able to die by euthanasia at St Paul's hospital rather than be transferred to St. John's Hospice to die.
Katie DeRosa reported for The Vancouver Sun on June 23
that Dying With Dignity and O'Neill's family initiated a campaign to
pressure the BC government to force Catholic hospitals to kill their
patients by euthanasia.
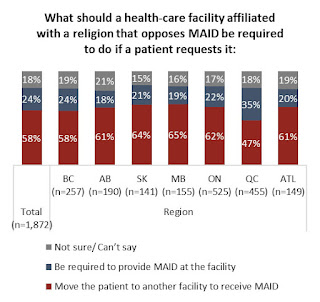
On October 17, 2023; an Angus Reid Institute poll indicated that 58% of Canadians believe that religiously affiliated healthcare should not be forced to provide (MAiD) euthanasia but should transfer the person to a facility that will provide euthanasia, while 18% of Canadians were unsure and only 24% of Canadians demanded that religiously affiliated healthcare facilities must provide euthanasia.The poll results varied by province with Manitoba (65%) and Saskatchewan (64%) offering the strongest support for religiously affiliated healthcare while Québec (47%) responded with the lowest support. Only 35% of the Québec poll participants stated that religiously affilitiated institutions must provide euthanasia.
The other key question in the Angus Reid Institute poll concerned conscience rights for medical professionals who oppose euthanasia. The poll found that 70% of Canadians thought that a medical professional who opposes euthanasia should refer someone who requests euthanasia to a medical professional who will provide it while 30% believed that medical professionals should not be forced to refer for euthanasia.
The Angus Reid Institute did not differentiate between a doctor being required to refer a patient for euthanasia or a doctor who opposes euthanasia being required to make an "effective referral" for euthanasia. Most medical professionals are willing to refer a patient, but not make an effective referral since an effective referral means sending the patient to a medical professional who will do the act.
Medical professionals who oppose euthanasia, usually oppose killing their patients. If they believe that its morallly wrong to kill a patient then they will also believe that its morally wrong to send their patient to someone who will kill their patient.
Nonetheless, Canadians clearly support the right of religiously affiliated healthcare institutions to not provide euthanasia.
An Angus Reid Institute poll that was published on September 28 found that only 28% of Canadians support euthanasia for mental illness alone. This is important because Canada is adding mental illness as a reason for euthanasia starting in March 2024.