"Those who believe that legal assisted suicide/ euthanasia will assure their autonomy and choice are naive."
William Reichel, MD
Montreal Gazette, May 30, 2010[1]
By Margaret Dore
January 26, 2012
A. Introduction
Leblanc vs. Attorney General of Canada brings a constitutional challenge to Canada's law prohibiting aiding or abetting a suicide. Leblanc also seeks to legalize assisted suicide and euthanasia as a medical treatment. In 2010, a bill in the Canadian Parliament seeking a similar result was overwhelmingly defeated.
Legalization of assisted suicide and/or euthanasia under Leblanc will create new paths of elder abuse. This is contrary to Canadian public policy. Legalization will also empower the healthcare system to the detriment of individual patients. There will be other problems.
B. Parliament Rejected Assisted Suicide and Euthanasia
On April 21, 2010, Parliament defeated Bill C-384, which would have legalized assisted suicide and euthanasia in Canada.[2] The vote was 228 to 59.[3]
C. The Notice of Civil Claim
In Leblanc, the Notice of Civil Claim seeks to strike down § 241(b) of the Criminal Code of Canada as contrary to the Canadian Charter of Rights and Freedoms.[4] § 241(b) states:
"Every one who . . . (b) aids or abets a person to commit suicide, whether suicide ensues or not, is guilty of an indictable offence and liable to imprisonment for a term not exceeding fourteen years."[5]
If § 241(b) would be struck down, it appears that any person, without restriction, would be allowed to assist another person's suicide.

The Notice of Claim also seeks to allow a healthcare professional, not necessarily a doctor, and/or a person acting under the professional's supervision, to "obtain and/or administer medication and/or the necessary treatment to end [the plaintiff's] life."[6] This request, to allow someone to actively administer a lethal modality to another person, is a request for euthanasia. The Canadian Medical Association states:
"Euthanasia means someone taking active measures to end life."[7]
In the context of traditional medical treatment, a person acting under the "supervision" of a healthcare professional would include a family member.[8] An example would be an adult child who administers medication to a parent under the supervision of a doctor who is not present.[9] This would typically be in a home setting.[10]
The Notice of Claim does not define any particular eligibility for assisted suicide/euthanasia other than a description of the plaintiff.[11] She is a disabled woman with ALS.[12]
D. A Comparison to the United States
In the United States, there are two states where assisted suicide is legal: Oregon and Washington.[13] The laws in these states were enacted via ballot initiatives, which are similar to a referendum in Canada.[14] No such law has made it through the scrutiny of a legislature despite more than 100 attempts.[15]
The Oregon and Washington laws apply to patients predicted to have less than six months to live, who are typically age 65 or older.[16] The statutes have safeguards, for example, two doctors are required to approve a lethal prescription; there are also waiting periods.[17] These laws nonetheless leave patients unprotected against elder abuse, coercion and even murder. Alex Schadenberg, executive director of the Euthanasia Prevention Coalition, states:
"With assisted suicide laws in Washington and Oregon, [elder abuse] perpetrators can . . . take a 'legal' route, by getting an elder to sign a lethal dose request. Once the prescription is filled, there is no supervision over the administration. . . . [E]ven if a patient struggled, 'who would know?'" [18]
E. Elder Abuse
Preventing elder abuse is official Government of Canada policy.[19] Elder abuse includes physical, psychological and financial abuse.[20] Financial abuse is the most commonly reported type.[21] Elder abuse is, however, largely unreported and can be very difficult to detect.[22] This is due in part to the reluctance of victims to report. The Government of Canada website states:
"Older adults may feel ashamed or embarrassed to tell anyone that they are being abused by someone they trust."[23]
Will Johnson, MD, echoes these themes as follows:
"I see elder abuse in my practice, often perpetrated by family members and caregivers. A desire for money or an inheritance is typical. To make it worse, the victims protect the perpetrators. In one case, an older woman knew that her son was robbing her blind and lied to protect him. Why? Family loyalty, shame, and fear that confronting the abuser will cost love and care. . . .
Under current law, abusers take their victims to the bank and to the lawyer for a new will. With legal assisted suicide, the next stop would be the doctor’s office for a lethal prescription. How exactly are we going to detect the victimization when we can’t do it now?"[24]
If assisted suicide and/or euthanasia are legalized via Leblanc, new paths of abuse will be created against the elderly, which is contrary to Government of Canada public policy. For this reason alone, the relief requested in Leblanc should be denied.
F. Empowering the Healthcare System
In Oregon, where assisted suicide has been legal since 1997, patients desiring treatment under the Oregon Health Plan have been offered assisted suicide instead.[25] The most well known cases involve Barbara Wagner and Randy Stroup.[26] Each wanted treatment.[27] The Plan offered them suicide instead.[28]
Neither Wagner nor Stroup saw this scenario as a celebration of their "choice." Wagner said: “I'm not ready to die.”[29] Stroup said: “This is my life they’re playing with.”[30]
Wagner and Stroup were steered to suicide. Moreover, it was the Oregon Health Plan, a government entity, doing the steering. If assisted suicide and/or euthanasia are legalized in Canada, the Canadian health care system will be similarly empowered. Indeed, even the plaintiff could find herself pushed to her death before she is ready. She could be a Canadian "Barbara Wagner." Her "choice" would be compromised and/or denied.
F. Suicide Contagion.
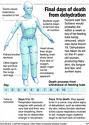
Oregon's suicide rate, which excludes suicides under its physician-assisted suicide law, has been "increasing significantly" since 2000.[31] Just three years prior, Oregon legalized assisted suicide.[32] This increased suicide rate is consistent with a suicide contagion.[33] In other words, legalizing one type of suicide encouraged other suicides. In Canada, preventing suicide is a significant public health issue.[34]
G. Conclusion
In Leblanc, the relief requested should be denied.
***
 |
| Margaret Dore |
Margaret Dore is President of Choice is an Illusion, a nonprofit corporation opposed to assisted suicide and euthanasia with a focus on the US and Canada. In November 2010, she appeared as an expert witness before the Select Committee on Dying with Dignity of the National Assembly of Quebec, Canada. She was an amicus curie in Baxter v. Montana, which is similar to Leblanc v. Attorney General of Canada.
Ms. Dore has been licensed to practice law in Washington State since 1986. She is a former Law Clerk to the Supreme Court of the State of Washington. She worked for the United States Department of Justice for one year. She has published multiple articles on elder abuse topics and against assisted suicide and euthanasia.
For more information, see:
http://www.choiceillusion.org/ and
http://www.margaretdore.com/.